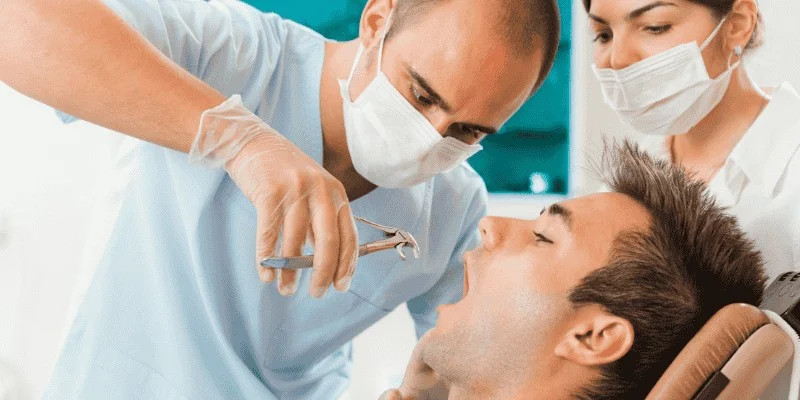
Most people assume any dentist can pull a tooth without issues. While general dentists handle many extractions successfully, specialists for tooth extraction require the advanced training that only an oral surgeon provides.
If your tooth is impacted, broken below the gumline, positioned near vital nerves, or you have complex medical conditions, you’ll likely need a specialist for safe removal.
Knowing when tooth extraction requires an oral surgeon helps you avoid complications and ensures proper care from the start.
Your regular dentist will evaluate your specific case and refer you to a specialist when needed. The decision depends on factors like tooth position, root structure, infection severity, and your overall health.
Understanding the difference between routine and complex extractions gives you confidence in your treatment plan. This guide explains exactly when specialist care becomes necessary and what to expect during the process.
Key Takeaways
- Impacted teeth, severe fractures, and proximity to nerves typically require an oral surgeon’s expertise
- Oral surgeons complete 4-6 years of additional surgical training beyond dental school
- Complex medical conditions like bleeding disorders or heart disease often need specialist-level precautions during extraction
Why Tooth Extractions Sometimes Require a Specialist
Some teeth need more than basic removal techniques due to their position, structure, or surrounding complications. When standard tools and methods aren’t enough, your general dentist may recommend working with an oral surgeon who has advanced training in complex cases.

Complex Tooth Anatomy
Your tooth’s shape and position can make removal challenging for a general dentist. Teeth with curved or multiple roots require careful sectioning to avoid breaking during extraction.
Impacted wisdom teeth that haven’t fully emerged through the gums often grow at angles or remain trapped under bone.
When a tooth is fractured below the gumline, standard forceps can’t grip it properly. The tooth extraction specialist needs to make incisions in your gum tissue and sometimes remove surrounding bone to access the broken pieces.
Teeth located near nerves or sinuses also demand precise surgical techniques to protect these vital structures.
Some teeth develop unusual root formations that show up on X-rays. Your dentist may spot these irregularities during examination and determine that specialized surgical tools and expertise are necessary for safe removal.
Risk of Complications
Certain situations increase the chance of problems during tooth extractions. Deep infections that spread beyond the tooth into facial tissues require immediate surgical attention and possibly IV antibiotics. Oral surgeons are trained to handle these urgent cases with advanced infection control methods.
If you have a bleeding disorder or take blood thinners, you need extra precautions during the procedure. Dental professionals with surgical training can coordinate with your doctor to adjust medications safely.
Heart conditions and diabetes also require special protocols that oral surgeons routinely manage.
Previous failed extraction attempts make subsequent removal more difficult. The tooth structure may be compromised, and surrounding tissue could be damaged. A tooth extraction specialist has the experience to complete what a general dentist couldn’t finish safely.
Beyond the Scope of General Dentistry
General dentists handle straightforward tooth extractions daily, but their training has limits. Oral surgeons complete an additional 4-6 years of hospital-based surgical residency after dental school.
This extensive education covers complex surgical techniques, anesthesia administration, and management of medically compromised patients.
When you need IV sedation or general anesthesia, an oral surgeon provides this service in their office. They’re qualified to monitor your vital signs and respond to any complications during deeper sedation. Your general dentist typically only offers local anesthesia for routine procedures.
Some cases require specialized imaging like CBCT scans to plan the surgical approach. Oral surgeons use this technology to map out nerve locations and bone density before making the first incision, ensuring the safest possible outcome for your tooth extraction.
Types of Tooth Extraction Procedures
Dentists perform different extraction methods based on how accessible your tooth is and whether it sits above or below the gum line. The approach your dentist chooses depends on factors like tooth position, root structure, and surrounding bone density.
Simple Extractions
A simple extraction works for teeth that are visible in your mouth and can be removed without cutting into the gums. Your dentist numbs the area with local anesthesia and uses special tools to loosen and lift the tooth from its socket.
This procedure typically takes just a few minutes. Your dentist grasps the tooth with forceps and rocks it back and forth to widen the socket before pulling it out.
Simple extractions work best for teeth that aren’t broken below the gum line or severely damaged. You’ll feel pressure during the removal but shouldn’t experience pain thanks to the numbing medication.
Surgical Extractions
A surgical tooth extraction requires additional steps beyond what simple extractions involve. Your dentist or oral surgeon may need to make an incision in your gums, remove surrounding bone, or cut the tooth into smaller pieces for removal.
This approach becomes necessary when teeth break at the gum line, have curved roots, or sit in dense bone. Surgical extractions often use IV sedation or general anesthesia depending on the complexity.
The dentist creates a small flap in your gum tissue to access the tooth and surrounding bone. After removing the tooth, they close the incision with stitches that dissolve on their own or need removal after a week.
Impacted Wisdom Teeth Removal
Impacted wisdom teeth are third molars that can’t emerge normally through your gums. They may be trapped under gum tissue only, partially covered by bone, or completely encased in your jawbone.
Removing impacted teeth always requires surgical extraction techniques. Your oral surgeon makes an incision to expose the tooth and removes any bone blocking access.
Types of impaction include:
- Soft tissue – tooth covered only by gums
- Partial-bony – upper portion partially surrounded by bone
- Full-bony – tooth completely encased in jawbone
The surgeon often cuts the tooth into sections to remove it piece by piece. This approach reduces the amount of bone removal needed and makes the procedure safer for you.
Common Scenarios Needing Specialist Care
Some tooth problems are too complex for a regular dentist to handle safely. When teeth have unusual positions, deep infections, or sit near important structures in your jaw, you’ll need someone with surgical training.

Severe Tooth Decay or Abscess
When tooth decay goes untreated for too long, it can destroy most of the tooth structure and spread infection deep into your gums and jawbone. An infected tooth often forms an abscess, which is a pocket of pus that causes severe pain and swelling.
Root canal treatment might save some infected teeth, but when the damage is too extensive, extraction becomes necessary. If your infection has spread beyond the tooth into your facial tissues or threatens your airway, you need surgical intervention from a specialist.
An oral surgeon can handle these situations because they’re trained to:
- Remove teeth that have broken apart from severe decay
- Drain infections that extend into surrounding tissues
- Administer IV antibiotics during the procedure
- Manage complications that arise during extraction
Deep infections require careful removal techniques since the tooth structure is often too weak to extract normally.
Fractured or Impacted Teeth
A tooth broken below your gumline can’t be removed with standard tools. Your dentist would need to cut into your gum tissue and possibly remove some bone to access the fractured pieces.
Impacted teeth are stuck under your gums and can’t come through normally. Wisdom teeth are the most common impacted teeth, but other teeth can become impacted too. These teeth may press against neighboring teeth, cause recurring infections, or develop cysts.
Removing impacted wisdom teeth often requires the surgeon to section the tooth into smaller pieces. This makes removal easier and reduces trauma to surrounding bone and tissue.
Curved or Multiple Roots
Your tooth roots anchor it into your jawbone. Most front teeth have single, straight roots that come out relatively easily. Back teeth often have multiple roots that can curve in different directions.
Curved roots make extraction tricky because they can break if pulled straight out. Molars typically have two or three roots, and each root might curve at a different angle. If imaging shows your tooth has unusual root anatomy, your dentist will likely refer you to a specialist.
An oral surgeon has the training to remove bone around curved roots or divide the tooth into sections. This approach prevents root tips from breaking off and staying trapped in your jaw.
Teeth Close to Sinuses or Nerves
Your upper back teeth sit very close to your maxillary sinuses. Your lower back teeth rest near the inferior alveolar nerve, which provides feeling to your lower lip and chin.
Removing teeth in these areas carries risks. You could end up with a hole between your mouth and sinus, or you might damage the nerve and lose sensation in part of your face.
Oral surgeons use special imaging like CBCT scans to see exactly where these structures are located. They know surgical techniques to protect nerves and sinuses during extraction. If complications do occur, they have the expertise to repair them immediately.
Patient Health and Medical Considerations
Your overall health plays a major role in determining whether you need a specialist for your tooth extraction. Certain medical conditions, medication use, and anxiety levels can increase risks during the procedure, making it safer to work with an oral surgeon who has advanced training.
Pre-Existing Medical Conditions
Medical conditions can complicate tooth extractions and create serious risks during the procedure. If you have heart disease, diabetes, or blood-clotting disorders, you need extra precautions that a specialist is better equipped to handle.
Heart-related conditions require special attention. If you have congestive heart failure, a history of heart attacks, or artificial heart valves, your body may struggle with the stress of surgery. You might need supplemental oxygen during the procedure or prophylactic antibiotics to prevent infection.
Diabetes affects how your body heals and fights infection. When your blood sugar is not well controlled, you face higher risks of complications. A specialist can schedule your extraction at the best time of day and monitor your glucose levels throughout the procedure.
Blood disorders like hemophilia or taking blood thinners create bleeding risks. You may need special management during oral surgery to control hemorrhaging. Specialists have the training and equipment to handle these situations safely.
If you have kidney disease, liver problems, or are undergoing cancer treatment, your dentist will likely refer you to a specialist who can coordinate with your medical team.
Use of Anesthesia or Sedation
Some patients require more than basic local anesthesia for their extraction. If you need sedation due to the complexity of your case or your anxiety level, a specialist is the safer choice.
Oral surgeons are trained to administer various sedation levels, from nitrous oxide to IV sedation. They monitor your vital signs throughout the procedure and can respond quickly to any complications. General dentists typically only use local anesthesia.
Your medical history affects which anesthesia options are safe for you. If you have respiratory conditions like asthma, heart problems, or take certain medications, these factors influence sedation choices. A specialist evaluates these risks more thoroughly.
Patients with sleep apnea or obesity may need special monitoring during sedation. Specialists have emergency equipment and training to manage breathing difficulties or other urgent situations that can arise.
Dental Anxiety and Comfort Management
Dental anxiety affects many people and can make tooth extractions more difficult. When your anxiety is severe, working with a specialist who offers sedation options helps you receive the care you need without extreme distress.
Specialists understand how stress impacts your body during oral surgery. High anxiety levels can raise your blood pressure and increase bleeding. They use anxiety-control methods to keep you calm and reduce physical complications.
IV sedation allows you to remain relaxed or even sleep through the procedure. You won’t remember the extraction, which helps if you’ve had traumatic dental experiences in the past. This option is particularly helpful for lengthy or complex extractions.
If you’ve fainted during previous dental work or have a strong gag reflex, a specialist can accommodate these needs better. They create a controlled environment where your comfort and safety are priorities throughout the entire process.
What to Expect from a Specialist Tooth Extraction
A specialist extraction involves careful planning, advanced techniques, and detailed aftercare instructions. You’ll go through an assessment phase, the surgical procedure itself, and a recovery period with specific guidelines to protect your oral health.
Initial Consultation and Evaluation
Your first visit focuses on understanding your specific situation. The oral surgeon will review your medical history and any medications you’re currently taking.
They’ll examine the tooth that needs to be pulled and take X-rays or a CBCT scan. This imaging shows the tooth’s position, root structure, and how close it sits to nerves or sinuses.
The surgeon will explain why you need a specialist extraction instead of a simple one. You’ll discuss anesthesia options like local numbing, oral sedation, IV sedation, or general anesthesia.
This is when you can ask questions about the procedure and recovery. The surgeon will also talk about tooth replacement options such as dental implants or dentures if needed. You’ll receive a cost estimate and schedule your extraction date.
Procedure Steps and Techniques
On the day of your extraction, the surgical team will start by administering your chosen anesthesia. Once you’re comfortable and numb, the surgeon begins the procedure.
For impacted or broken teeth, they’ll make a small incision in your gum tissue. They may need to remove some bone around the tooth to access it properly.
Common surgical techniques include:
- Sectioning the tooth into smaller pieces for easier removal
- Using specialized instruments to loosen the tooth from its socket
- Carefully extracting each section while protecting surrounding structures
- Placing stitches to close the incision site
The entire procedure typically takes 30 to 60 minutes depending on complexity. You won’t feel pain during the extraction due to the anesthesia.
Post-Extraction Care and Aftercare Instructions
Right after your tooth is pulled, you’ll bite down on gauze to control bleeding. The surgical team will give you detailed post-extraction care guidelines before you leave.
Your aftercare instructions will include:
- Keeping gauze in place for 30 to 45 minutes
- Applying ice packs to reduce swelling during the first 24 hours
- Taking prescribed pain medication as directed
- Avoiding smoking, drinking through straws, or spitting forcefully
- Eating soft foods and staying hydrated
You need to avoid disturbing the blood clot that forms in the socket. Dislodging this clot can cause dry socket, a painful condition that delays healing.
Gently rinse with warm salt water starting 24 hours after surgery. Brush your other teeth normally, but avoid the extraction site for the first few days.
Most people return to normal activities within three to seven days. Your surgeon will schedule a follow-up visit to check your healing progress and discuss tooth replacement options if appropriate.
Frequently Asked Questions
The cost of specialist tooth removal depends on several factors including procedure complexity and anesthesia type. Understanding when you need specialized care and how to recover properly helps ensure the best outcome for your oral health.
What factors determine the cost of having a tooth extracted by an oral surgeon?
The complexity of your extraction plays the biggest role in determining cost. A simple extraction costs less than a surgical one that requires cutting into the gum tissue or removing bone.
The type of anesthesia you receive also affects the price. Local anesthesia is the most affordable option, while IV sedation or general anesthesia increases the overall cost.
Your geographic location matters too. Oral surgery procedures in urban areas or regions with higher costs of living tend to be more expensive than those in smaller towns.
Whether you need additional procedures like bone grafts or tooth sectioning will add to your total bill. Your insurance coverage and the specific oral surgeon you choose also impact what you’ll pay out of pocket.
Is it necessary to see a specialist for a tooth with a previous root canal, or can a regular dentist handle the extraction?
Most teeth that have had root canals can be removed by your regular dentist without issue. Root canal treatment makes teeth more brittle, but this doesn’t always complicate extraction.
You might need a specialist for complex tooth extraction cases if your tooth has curved roots or broke during the removal attempt. A tooth that fractures below the gum line during extraction requires surgical techniques that oral surgeons are better equipped to handle.
Your dentist will evaluate the tooth and recommend a specialist if they anticipate complications. Some general dentists prefer to refer all root canal tooth extractions to oral surgeons as a precaution, while others handle straightforward cases themselves.
What are some potential reasons a dentist would refer a patient to a specialist for tooth extraction?
Impacted teeth are one of the most common reasons for referral to an oral surgeon. When teeth are trapped beneath your gums or jawbone, removing them requires surgical access and specialized training.
Your dentist might refer you if the tooth is positioned close to important nerves. Extractions near nerves like the inferior alveolar nerve carry a higher risk of nerve damage that oral surgeons are trained to minimize.
Certain medical conditions make extractions more complex. If you take medications like bisphosphonates or have bleeding disorders, you need the specialized care an oral surgeon provides.
Teeth with severely curved or fused roots can be difficult to remove using standard methods. Dense jawbone that makes extraction challenging is another reason your dentist might send you to a specialist.
A previous failed extraction attempt also warrants a referral. When complications arise during the first try, an oral surgeon has the skills and tools to complete the procedure safely.
What specific care should be taken after having a tooth extracted to ensure proper healing?
Avoid smoking, spitting, and using straws for at least the first few days after your extraction. These actions can dislodge the blood clot in your socket and lead to a painful condition called dry socket.
Stick to soft foods like yogurt, soup, mashed potatoes, and applesauce while you heal. Hard, crunchy, or chewy foods can irritate the extraction site and slow down recovery.
Take your prescribed pain medications as directed and apply ice packs to reduce swelling. Gentle rinsing with warm salt water after 24 hours helps keep the area clean.
Following your surgeon’s post-operative instructions is crucial for proper healing. Keep your head elevated when lying down and get plenty of rest during the first few days.
Watch for signs of infection like excessive swelling, fever, or severe pain that worsens after a few days. Contact your oral surgeon immediately if you notice any of these symptoms.
What are the implications of an impacted tooth, and why might this condition require specialized care?
An impacted tooth remains stuck in your jawbone or gums instead of erupting normally into your mouth. This happens most often with wisdom teeth but can affect other teeth as well.
Impacted teeth can cause pain, swelling, and infection in the surrounding tissues. They may push against neighboring teeth and cause crowding or damage to adjacent tooth roots.
Removing impacted teeth requires surgical techniques that go beyond what a simple extraction involves. The oral surgeon must make incisions in your gums and sometimes remove bone to access the trapped tooth.
Oral surgeons complete 4-6 years of additional hospital-based surgical training after dental school. This specialized education prepares them to handle the complexities of impacted tooth removal safely.
The tooth may need to be sectioned into smaller pieces for easier removal. Sutures are typically required to close the gum tissue after the procedure is complete.
What are some reasons you might want to avoid tooth extraction, and what alternatives could a specialist provide?
Losing a tooth creates a gap that can affect your bite and cause neighboring teeth to shift over time. The bone in that area will also gradually deteriorate without a tooth root to stimulate it.
Dental implants offer a long-lasting replacement option that functions like a natural tooth root. Oral surgeons can place these artificial roots during the same visit as your extraction in some cases.
Root canal treatment might save a severely decayed or infected tooth. If your tooth structure is still intact enough, this procedure eliminates the infection while preserving your natural tooth.
A bone graft performed at the time of extraction helps preserve the jawbone for future implant placement. This preventive step maintains the bone volume you’ll need if you decide on an implant later.
Bridges and partial dentures are other options for replacing missing teeth. Your oral surgeon can discuss which tooth replacement option best fits your needs, budget, and long-term oral health goals.